Dear Doctor: I’m taking insulin and can’t seem to lose any weight. Why is it so difficult?


Answer provided by Robert Kushner, MD
Spring 2016
If the title of this article speaks to you, then you are one of 29 million people in the United States who has diabetes. Chances are that you have type 2 diabetes, which accounts for an estimated 90-95 percent of all diabetes cases. I’ll also bet that you are having difficulty managing your weight, since obesity is one of the strongest risk factors for developing the disease. In fact, the link between diabetes and obesity is so strong that many have called the combination of the two diseases “diabesity.”
The unintended consequences of some medications used to treat diabetes, like insulin, may cause additional weight gain. Fortunately, newer medications for the treatment of diabetes have been developed that do help with weight-loss. This article will provide a brief review of diabetes and the treatment options available. By reading this article, you will be better informed to have a conversation with your healthcare provider about selecting the best treatment for you.
What is type 2 diabetes?
Type 2 diabetes occurs when your pancreas is not able to produce enough insulin to overcome the resistance caused by excess body fat. The higher the resistance, the more the pancreas has to work. Throughout time, the pancreas becomes exhausted and cannot keep up. Insulin is needed to allow your blood sugar, or glucose, to enter the cells throughout the body.
If insulin cannot do its work, glucose starts to build up in the bloodstream. When the blood sugar level reaches 126 mg/dl, or the hemoglobin A1c (a long-term measurement of glucose control) exceeds 6.5 percent, then a diagnosis of diabetes is made. Since diabetes is a life-long disease and can damage your heart, eyes and kidneys, it is important to seek treatment with a healthcare provider.
How do I begin to take charge of my diabetes?
Achieving a healthy body weight and engaging in daily physical activity is the cornerstone of diabetes management. As little as a three to five percent of weight-loss can have remarkable effects on improving your blood sugar and reducing health complications linked to type 2 diabetes. In addition to reducing your dietary calories to achieve weight-loss, it is also important to limit your carbohydrate intake, particularly carbohydrates found in sugars in bakery goods, snacks and sugar-sweetened beverages.
You should also set a goal of achieving 150 minutes of physical activity each week, which can be achieved by taking a 30 minute brisk walk, five days a week. This will help push the blood sugar into your muscles. Patients who are diagnosed with diabetes are also recommended to see a registered dietitian for personalized lifestyle guidance.
When do I need to take medication to treat my diabetes?
Although it is important to follow a healthy diet, increase physical activity and engage in weight management, medication is commonly needed to help control your blood sugar. Determining when it’s time to add medication will depend on how high your blood sugar is, how effective lifestyle management strategies have been and the status of your overall health.
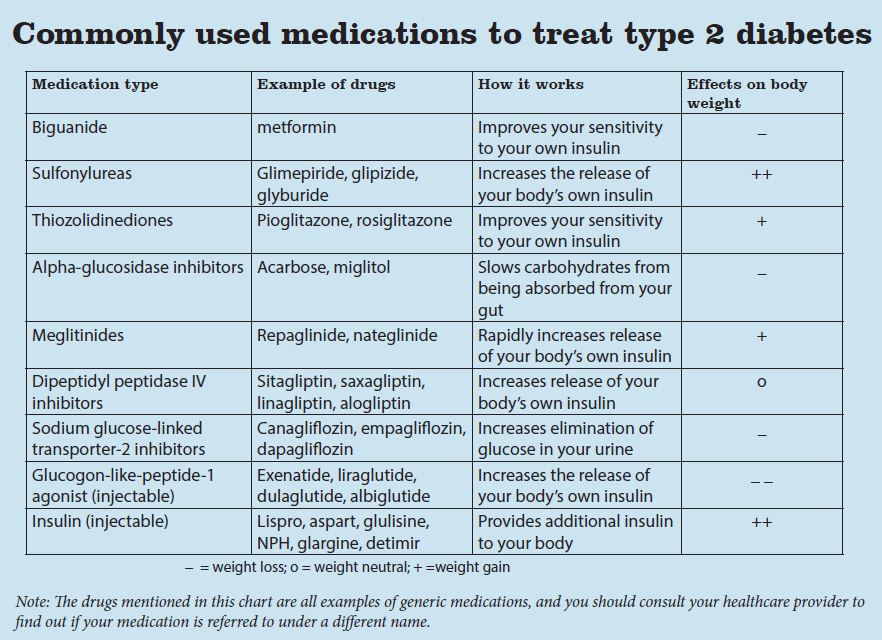
There are nine different classes of drugs to choose from, and they are often used in combination to increase effectiveness since they work in different ways.
How does my healthcare provider choose which medication to prescribe?
The first medication used is usually metformin due to its history of effectiveness, use, safety, tolerability and cost. This medication is also commonly associated with modest weight-loss, and that weight-loss is often continued throughout the course of treatment.
If a second medication is needed to better control the blood sugar, your healthcare provider has multiple options based upon each medication’s effectiveness, cost, side effects, your lifestyle and your personal preferences. Since diabetes is a long-term disease, many patients will need two or three medications to control their body’s blood sugar throughout their life.
With the understanding that obesity is a disease and a significant contributing factor to diabetes, many providers are now preferentially choosing medications that are weight neutral or cause weight-loss instead of selecting those that cause weight gain. The effect on body weight for each drug is listed in the table.
Your healthcare provider will take multiple factors into consideration before considering prescribing insulin, one of the most effective treatments for diabetes.
The primary reason for choosing insulin is uncontrolled diabetes despite using one, two or multiple oral medications. Although quite effective, insulin needs to be injected once or sometimes several times a day, and it poses a risk of causing patients to develop low blood sugar (hypoglycemia) and gain weight. The use and side effects of insulin are always discussed prior to beginning treatment so that you can be prepared.
If my healthcare provider prescribes insulin, how can I control my weight?
Weight gain is a common side effect of insulin. This is due in part to the improved control of diabetes and the increased uptake of sugar into cells in your body. Weight gain may also occur as a result of hypoglycemia. When your body’s blood sugar goes too low, you may experience weakness, lightheadedness, dizziness or a rapid heartbeat.
The treatment is to bring your blood glucose levels up quickly by taking in “quick-fix food” that is equal to 15 to 20 grams of sugar or carbohydrates, such as 1/2 cup of fruit juice, four or five saltine crackers, or two tablespoons of raisins. If this occurs frequently, patients may deliberately increase their calorie intake to avoid the symptoms. Although everyone is different, weight gain from insulin frequently ranges anywhere from four pounds to more than 13 pounds.
Taking a weight-losing diabetes drug along with insulin can limit the weight gain, but it is also important to follow a calorie-controlled diet and engage in daily physical activity. The long-term goal is to keep the insulin dose as low as possible depending upon the control your body has of the diabetes.
Take Home Messages
- Diabetes is a major cause of illness and earlier death rates. Gaining weight and being affected by excess weight or obesity increases the chances of being affected by type 2 diabetes.
• As little as a three to five percent weight-loss can have a significant effect on controlling the disease.
• There are nine classes of drugs that are approved by the FDA for type 2 diabetes treatment, many of which have the effect of weight-loss in addition to improving the blood sugar.
• Weight gain is commonly seen with insulin use, which can be partially controlled by taking a weight-loss medication at the same time, and by following a healthy lifestyle plan.
About the Author:
Robert Kushner, MD, is a passionate clinician, educator, researcher and advocate in helping to improve the lives of those affected by excess weight and obesity. Dr. Kushner is the Medical Director of the Center for Lifestyle Medicine at Northwestern Memorial Hospital in Chicago and Professor of Medicine, Northwestern University Feinberg School of Medicine, and is also on the OAC’s National Board of Directors. Dr. Kushner believes in the power of lifestyle to improve health and body weight. With a background in nutrition and behavior change, he has dedicated his career to personalizing weight-loss diet and treatment plans to meet the needs of each person.
Dr. Kushner will also be speaking at the 5th Annual Your Weight Matters National Convention during the following sessions: “360 Degrees of Movement: Integrating Activity and Exercise into Your Day,” and “The Struggle is Real – Why is it so Hard to Manage My Weight?” To contact Dr. Kushner or for more information about his work, visit www.drrobertkushner.com.
by Sarah Ro, MD; and Young Whang, MD, PhD Fall 2023 Mary, a postmenopausal woman with a…
Read Articleby Rachel Engelhart, RD; Kelly Donahue, PhD; and Renu Mansukhani, MD Summer 2023 Welcome to the first…
Read Articleby Sarah Bramblette, MSHL Summer 2023 In the final months of 2022, I experienced both the worst…
Read Article








