Why Aftercare is Not Optional for Long-term Success


by Jill C. Williams, MS, CPT
Winter 2014
Obesity surgery, regardless of procedure choice, is a gift. I don’t mean that in the traditional sense of the word. You, your insurance carrier or a combination of both paid for the surgery. The gift is the procedure itself.
There are many more choices for bariatric (obesity) surgery now than in 1998 when mine was done, and this article is not about any specific surgery. Along with your medical care team, you made (or will make) a decision for a particular surgery based on your general health, any obesity-related co-morbidities and what procedures your medical insurance provides coverage for according to your policy. We come to this point in our lives with a variety of expectations, at a variety of ages and live our lives on very different playing fields. So, this article focuses on what happens next – YOUR life post-surgery.
About Me
A bit about my history: I had a duodenal switch procedure in 1998; with a starting weight of 330 pounds, Type 2 diabetes, sleep apnea and high blood pressure. I was on a c-pap machine for the apnea and on oral medications for the others. As of now, I am 135 pounds, no obesity-related comorbidities and am a happy and healthy 59-year-old. I have undergone several rounds of plastic surgery (some covered by insurance; some not) and am living a great life.
I have seen and or heard of many people go through a surgical procedure, do well for a while, and they either quickly or slowly regain their weight. A small percentage of this can be traced back to a physical cause related to the surgery or a new illness; for the most part, weight regain is lack of support and a strong program that routinely encourages high quality self-care. That is one of the glaring issues with any obesity surgery, it is a tool; it is not a cure. If we make no behavioral changes, no commitment to a new way of life and health and do not take the time to nourish ourselves well, then weight gain is almost inevitable.
My Weight-loss Journey
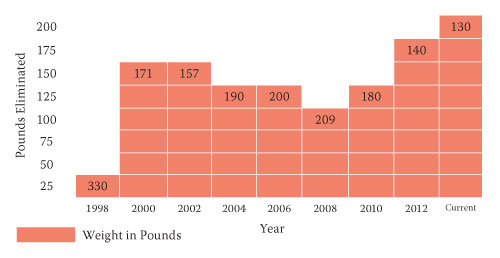
My own weight-loss history is fairly straightforward, good weight loss with a period of coasting for about six years where my weight was not ideal; but “not bad.”
Keys to Success
As statistics show in the research available, many people do quite well in their first year(s) following their procedures. This is partly our adjustment to the surgery, partly our enthusiasm for success and our high levels of self-motivation. In my own course of research (non-scientific); I have found that like me, many people have settled into a comfort zone. While not at their ideal weight, they are significantly lighter, may have gotten rid of several comorbidities and their surgeon is pleased with the progress!
The key to all of this is that if you want the best results, you must have a large amount of control over your long-term success. You can choose to add into your journey any of the below resources that are key to this success:
Support from Your Surgeon and Healthcare Provider
Your surgeon or provider will be able to help you learn more about nutrition & supplementation. Annual blood tests are needed with malabsorptive procedures, and all quality surgical practices have an aftercare program to support your medical needs. Your surgeon and your primary care physician will guide you to long term success in the medical arena. Your medical team can tell you what you “should” eat and how best to maximize your weight-loss and improve your health – the decision to actually do that remains with you. These surgically-based support groups also provide great information to family members and most have a small amount of active emotional support with each patient forming relationships with other post-ops to provide more encompassing emotional support.
Support from Your Family/Friends
Family support is particularly important to having long term success. Be sure that you and your family and friends understand what you will be experiencing from a medical perspective, and have as much open communication as possible before and after your procedure. Weight-loss impacts many areas of your life (what you eat, how you move, your physical appearance, your sexual relationships, your spousal relationship, work relationships, etc.), and it is essential to understand your own needs and be able to communicate them. In some instances, family and friends are used to us being affected by obesity, and they feel like they are losing us with our weight-loss. Here again, open communication is essential.
Support from a Therapist
For some of us, our weight has been an issue for so long that the rapid weight-loss brings up unresolved issues and feelings that are best sorted out with a therapist or counselor. Although most surgical practices require a psychological screening prior to surgery, be sure that you have resources lined up if your screening shows that you may want some additional support in this arena. Weight-loss only makes you thinner; it does not eliminate emotional, addictive or psychological issues. You may also find it useful to undergo some therapy as a family to be sure that all family members are on the same page in terms of what success means to YOU!
Support from a Fitness Trainer
Whether in a pre-op stage or newly post-op, most of us did not excel at exercise during our time of weight gain or obesity. For some, it is embarrassing to go to a gym. For others, it is a financial struggle to pay for a membership or training. For some, we simply want the surgery to be the CURE and not have to work so hard! Fitness and movement need to become a part of your life for long term success. Trust me, it is vastly easier and more enjoyable to have workouts and partake in high energy events (hiking, biking, etc.) at 130 pounds. I was one of the embarrassed ones and simply stopped exercising. I returned to a gym environment (aqua aerobics and elliptical trainer) in addition to simply walking more during my first year. Do what you can; but DO SOMETHING! You will need to redefine this area of life; set goals and work toward what will become your standard of fitness for you! Some trainers will work in outdoor settings, some will come to your home, some will have their own facilities or work with an established local health club. If you think this would be helpful, find the right trainer and go for it! If this is not an option, buddy-up with another post-op that lives close by (perhaps someone from your surgery support group) and make play dates together. Get out and move and have fun!
Support from a Coach
Again, I realize this can be a costly venture, and I recommend you find an aftercare program that combines 1:1 coaching with fitness and group support as a great and perhaps more economical resource. Ask your surgeon to recommend one in your community, do some research on the Internet, and I am also happy to help you find local resources. Coaching differs from therapy in that it assumes an emotionally healthy, resourceful and creative person who wants to take charge of their lives. You will set the agenda, choose your goals, and together with your coach, will reach successful outcomes or examine why you did not. Coaching is not about blame/failure, etc. It is about holding yourself accountable for your life, in the present and future. While therapy can help you deal with your past, coaching is very much a NOW activity and should be approached that way. Be sure to find an appropriately certified coach as there are currently few regulations about who can call themselves a coach. If you want further information, please feel free to contact me.
Support from a Food Plan
For some, our eating will continue to be an issue, and I know that people have found the structure of commercial weight-loss programs both emotionally supportive and a healthy way to give their food plan some boundaries. For me, the key has been the elimination of simple carbohydrates (all sugars, any products made with flour), and I have a very peaceful relationship with food and easily maintain my current weight. Again, the surgery is a TOOL, not a cure, so seeking other forms of support is perfectly normal and healthy!
I have been involved with any combination of the resources on page 50 throughout the years and have found significant help from each depending upon the current issue and how much time and money I had to seek external support. Through journaling, prayer and a lot of talking to myself and others, I was able to solidify these things for myself about my life going forward:
- I needed to forgive myself for past mistakes and reclaim ownership of my life and my body.
- I wanted to be able to enjoy and trust my body to work physically.
- I wanted to make peace with food.
- I wanted to find my purpose NOW, not the one that was relevant at 25 or 45, but the life I wanted at 56 and beyond.
As I move forward the most important thing comes down to my attitude, how I frame my life and the language I use for my internal talks. With any food plan, I have a choice of how I view things. Notice the language; “I chose to eliminate…” rather than “I am forcing myself to give up…” – HUGE difference in self talk, and HUGE difference in my attitude and success! Reframe the gym into an adult playground and stop exercising and start playing!
Repeat after me: IT IS NEVER TOO LATE TO WRITE MY NEXT JUICY LIFE CHAPTER!
I tell you these things not to promote a particular surgery, food plan or aftercare choice. I tell you these things so that you too can go and find YOUR way, YOUR path and YOUR bliss. The surgery helps to change your weight; YOU are ultimately in charge of your life. My advice is to honor who you are.
My wish for you is that you have:
- Courage to seek out and obtain support
- An attitude of gratitude about the surgery and life itself
- Success in your endeavors!
Conclusion
You can find all that you need for life-long success with your weight. Find the courage to ask for what you need and accept nothing less. Yet another lesson: I don’t get everything I want, AND I create a life where I get everything I need. As with any gift, treasure your opportunity to have obesity surgery and commit to taking great care of yourself.
About the Author:
Jill C. Williams, MS, CPT, is a wellness coach, certified personal trainer and workshop facilitator. Jill had a DS procedure in 1998 and has gone from 330 pounds to 130 pounds. She is an obesity surgery aftercare program developer and works with individuals and small groups to ensure long-term success through fitness training, wellness coaching and group support. She is a tireless advocate for helping you create a body you love and trust physically and emotionally.
by Kendall Griffey, OAC Communications Manager Spring 2024 We have officially kicked off Your Weight Matters Regional…
Read Articleby Robyn Pashby, PhD Winter 2024 “No one is ever going to date you if you don’t…
Read Articleby Kendall Griffey, OAC Communications Coordinator Winter 2024 The Obesity Action Coalition’s 12th annual Your Weight Matters…
Read Article









