Weight-Loss Surgery Treatment Options


Summer 2006
Introduction
In this issue of OAC News, the Cover Story provides you with an in-depth explanation of the three most commonly selected weight-loss surgeries:
- Roux-en-Y Gastric Bypass
- Laparoscopic Adjustable Gastric Banding
- Biliopancreatic Diversion with Duodenal Switch
Weight-loss surgery, also commonly known as bariatric surgery, is a safe and effective treatment option for those affected by morbid obesity. Morbid obesity is defined as having a body mass index (BMI) greater than 40, or weighing more than 100 pounds over ideal body weight. In addition, a patient with a BMI greater than 35 with one or more obesity-related diseases is classified as severe obesity.
There is a great amount of importance and responsibility associated with choosing a weight-loss treatment option. Weight-loss surgery is one of the most commonly chosen and performed treatment options for morbid obesity; however, choosing which surgery is right for you can be a difficult task. This article will provide you with the education needed for you and your physician to make the appropriate treatment selection. Consult your physician and insurance provider to see if you are a candidate.
Remember, weight-loss surgery is not the “easy way out.” This treatment option is a tool that you will continually use to lose weight. Surgery is a resource to help you reduce your weight. Behavioral, physical and psychological changes are required for you to maintain a healthy quality of life. Continued positive weight-loss relies upon your desire and dedication to change your lifestyle with a proactive approach.
In the Cover Story, you will see terms, such as “Malabsorptive” and “Open,” that you may not be familiar with. Prior to reading about the different surgeries, we have provided you with a brief description of some of the most commonly used terms.
Open vs. Laparoscopic
In each section, you will see the surgeries described as being performed “Open” or “Laparoscopic.” Although laparoscopic has increasingly gained in popularity and frequency, “Open” is also still commonly used in practice today.
“Open” – The Open approach procedure involves a long incision that opens the abdomen, which provides the surgeon access.
“Laparoscopic” – In Laparoscopic surgery, a small video camera is inserted into the abdomen allowing the surgeon to conduct and view the process on a video monitor. Both camera and surgical instruments are inserted through small incisions made in the abdominal wall.
Malabsorptive vs. Restrictive
Throughout the Cover Story, the surgeries will be described as “Malabsorptive” or “Restrictive.” Depending on the type of procedure that is determined to be best for your needs, each form requires different lifestyle changes.
“Malabsorptive” – Malabsorptive procedures alter digestion, thus causing the food to be poorly digested and incompletely absorbed.
“Restrictive” – Restrictive procedures decrease food intake by creating a small upper stomach pouch to limit food intake.
In addition to these terms, there may be other words, topics or descriptions that you might not understand. If so, make sure to speak with your physician further to gain a better understanding.
Weight-Loss Treatment Options
As you begin reading, remember, weight-loss surgery is a tool to help you lose weight. As weight-loss surgery is a commitment for life, it is imperative that you educate yourself about your treatment choice and have the appropriate support system in place to help you with your journey ahead.
Gastric Bypass Roux-en-Y
By Robin Blackstone, MD, FACS, and Melissa Davis, RN, MSN, ANP, APRN-BC, CNS
|
Gastrointestinal Tract after |
 |
| ©2003-2006 Endo-Surgery, Inc. All rights reserved. Used by permission |
Worldwide, the gastric bypass Roux-en-Y is the most frequently performed obesity operation and accounts for 85 percent of all bariatric surgery in the United States.
It is unique in that it is the first of the gastric procedures for morbid obesity to combine restriction with malabsorption. Also, there is an element of intolerance for many patients. These three elements are what make the gastric bypass Roux-en-Y so popular and effective in creating a tool for successful, long-term weight-loss, and resolution of the co-morbidities associated with morbid obesity.
The gastric bypass Roux-en-Y can be performed by both open and laparoscopic techniques. It has been argued that there are advantages to both approaches, but these advantages seem to be related to the surgeon’s capabilities and skill sets, and not the patient’s recovery, surgical outcomes or resolution of co-morbidities. In the U.S., the laparoscopic technique has become the more popular approach by patients and competent surgeons, as recovery is quicker and post-operative wound healing complications are significantly reduced.
The gastric bypass Roux-en-Y surgery itself can be described in three significant steps. Each of these steps can be related directly to either restriction, malabsorption or intolerance.
1) creation of the pouch
2) creation of the jejunostomy
3) and the anastomosis of the jejunum to the pouch (the gastro-jejunostomy)
Often, the first step in the gastric bypass Roux-en-Y is the creation of the pouch. Restriction is produced because of the pouch. Restriction is one of the most significant outcomes of the surgery and is only related to volume of food able to be ingested at one sitting. This is what is achieved after the creation of a small gastric pouch with a small outlet that, with distention from eating food, causes the sensation of fullness.
The pouch can be created either horizontally or vertically, and is generally an average of 15 ml (one half of a shot glass) in capacity. This 15 ml is the size of the pouch initially, but because of the nature of stomach tissue, will eventually stretch to approximately the size of a small egg. Also, this is the size of the pouch at rest, which means that it is not the only amount of food that can be eaten at one time. The nature and texture of the food eaten at the time will determine volume of food eaten at each sitting. Although this initial small size of the pouch can create some challenges for the newly recovered gastric bypass patient, it’s creation is necessary in order to avoid a pouch that is later too large, preventing a patient from either reaching goal weight or being able to maintain long-term weight-loss.
The next step is the creation of jejunostomy, causing malabsorption. The malabsorptive element is created from the bypassing of the distal stomach, the entire duodenum and a distance of approximately 100 to 150 cm of the jejunum. A connection and opening are also made so that that food can be passed through the intestine and still receive the same digestive enzymes from the pancreas and liver. This connection is called the jejuno-jejunostomy. The malabsorptive element is significant to the bariatric patient, requiring vitamin supplementation; however, this element does not seem to be as significant in regard to long term weight-loss as the element of restriction.
The third step in the gastric bypass Roux-en-Y is the creation of the gastro-jejunostomy. During this step, the second part of the small intestine, the jejunum, is connected to the pouch. This connection is called the gastro-jejunostomy, and it is because of this connection between the pouch and the jejunum that a patient can experience intolerance.
This intolerance is in relation to certain foods, and is often referred to as “dumping” or “dumping syndrome.” This intolerance is a direct result of the food, usually higher in sugars and starches, entering directly into the jejunum having only mixed with saliva and not stomach acid. The symptoms of dumping syndrome may vary from person to person, but can include the following:
Although dumping syndrome may not seem desirable, it can be. For the gastric bypass patient, it can be a strong motivator to eat healthier, protein-dense foods and to avoid junk food. This has been referred to as “forced behavior modification.”
Many patients wonder what happens to their old stomach or if the rest of it was removed. What they are referring to is the distal portion of the stomach, or the part of the stomach tissue that was separated from the tissue used to create the pouch. The “old” or “distal” stomach is not removed, as this would not be in a patient’s best interest. First of all, it is still well connected to other organs in the body, and separating or removing it would provide an added risk.
Secondly, although the distal stomach will no longer receive food, it does continue to serve an important function. After gastric bypass, it still continues to receive digestive enzymes from the pancreas and liver, which are very necessary for digestion and absorption of nutrients. These enzymes continue to drain into the distal stomach, and flow through the duodenum, later mixing with food at the point where the food drains from the pouch and flows through the jejunum (jejuno-jejunostomy).
Weight-loss
Weight-loss after gastric bypass surgery usually exceeds 100 pounds, or can be anywhere from 65 percent to 100 percent of excess body weight. Weight-loss generally levels off after approximately one to two years, and a weight gain of up to 20 pounds is common. Long-term follow-up with a multidisciplinary program can usually provide the best weight-loss results.
Complications
Short term complications include pulmonary emboli, anastomotic leak, bleeding and wound infection. Operative (30 day post-op) mortality is about 0.5 percent. This means that approximately one out of every 200 patients who have gastric bypass will die within 30 days of their surgery. Patients need to remember that this number is what is reported nationally, and they should inquire with their individual practice as to their own mortality rate. Laparoscopic approach provides a shorter hospitalization stay, lower wound complication rate and a higher rate of postoperative patient comfort.
Long term complications can include stricture (generally the gastro-jejunostomy), ulcers, staple line disruption and internal hernia. Nutritional complications are few, and can generally be avoided with life-long supplementation of a multivitamin, iron, calcium and B12. Peripheral neuropathy is also a rare complication, and can mostly be avoided with vitamin supplementation and adequate protein intake. Also, ventral hernia rates are significant with open gastric bypass Roux-en-Y, just as for any open abdominal procedure.
Conclusion
All surgeries contain a certain level of risk. Be sure to speak with your physician to determine which weight-loss treatment option best fits your needs.
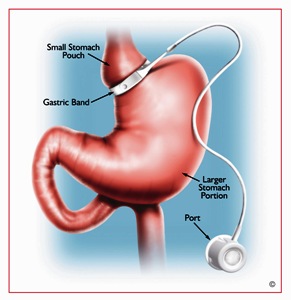
Laparoscopic Adjustable Gastric Banding
By Lloyd Stegemann, MD
|
Gastrointestinal Tract after |
 |
| ©2003-2006 Endo-Surgery, Inc. All rights reserved. Used by permission |
Obesity rates in the United States continue to rise. It is estimated that approximately 30 percent of Americans are affected by obesity and recent data suggests that we may actually be underestimating this number. As body weight rises, so does the incidence of serious medical problems related to the weight, such as diabetes, high blood pressure and sleep apnea.
The good news is that with weight-loss many of these medical problems improve or go away completely. The bad news is that this weight-loss is often difficult to achieve, especially for those who are significantly overweight. For many people, weight-loss surgery provides the best opportunity to achieve meaningful, sustained weight-loss. This article will focus on one of the most commonly selected weight-loss surgeries, the adjustable gastric band.
General Information
Currently, in the U.S., there is only one adjustable gastric band on the market (LAP-BAND®) although several different types of bands are available worldwide. The operation is almost exclusively done laparoscopically (minimally invasive). The adjustable gastric band is a purely restrictive weight-loss operation, meaning that it works by limiting the amount of calories (i.e. food) a person can take in. Unlike a diet, however, individuals still feel “full” with this reduced intake.
How It Works
This operation involves placing a silastic “belt” around the upper part of the stomach. The “belt” essentially separates the stomach into two parts: a tiny upper pouch and a larger lower pouch. The band is connected by tubing to a port or reservoir that sits below the skin of the abdominal wall usually around the belly button (the port site varies widely by surgeon). The port can’t be seen (and often can’t be felt) from the outside. Inside of the “belt” is a balloon that can be filled by placing fluid through the port. As the balloon is filled, it slows the passage of food from the upper pouch into the lower pouch. As the band is progressively filled, patients will feel “full” with smaller amounts of food. Typically patients will need two band fills before they feel significantly restricted and four to six band fills total in the first year after surgery.
Weight-loss & Health Benefit
Weight-loss with an adjustable gastric band is typically slow and steady. Band patients generally lose one to two pounds per week during the first year after band placement. Weight-loss can be seen for two to three years after surgery and most patients will eventually lose 50 to 60 percent of their excess weight.
Band patients often see a significant improvement in their weight related medical problems. Most patients will see a reduction in their need for medications to treat diabetes, high blood pressure, and high cholesterol and in fact many will come off of their medicines completely. Many patients will see resolution of their sleep apnea and will no longer have to sleep with a CPAP machine. Most patients also report a significant improvement in the quality of their life, as they are able to do activities they haven’t been able to do for years.
Advantages
There are several features that make the adjustable gastric band appealing. There is minimal stress to the body at the time of surgery because the band is almost always done laparoscopically and does not involve cutting the stomach or rerouting the intestines. Most patients can go home the same day or the next morning.
Recovery from surgery is usually quick and most people return to work a week or so after surgery. The risk of death from band surgery is 0.1 percent, although many centers report even lower rates.
The adjustability of the band makes it unique among weight-loss operations. This feature makes it possible to make band adjustments based on the individual weight-loss goals and needs of the patient. The stomach and intestines aren’t bypassed, so vitamin, mineral and nutrition problems after banding are unusual, but still possible. Many programs still recommend vitamin supplementation after banding.
The adjustable gastric band can be easily removed if necessary. Clearly we are learning more and more about obesity every day and there may come a time when medical management proves to be very effective in controlling weight. Band patients could have their band removed at that point and their gastrointestinal tract returned to normal.
Considerations Before Choosing A Band
Patients contemplating adjustable gastric banding must be comfortable with the thought of having a “foreign body” in them for life. Although no problems have been reported to date, it is unknown what the effect of having this foreign body will be in 20 to 30 years. It is also unclear at this point what the long-term (more than 10 years) weight-loss results with this operation will be, although the early data is promising.
After banding, patients need to be available for regular follow-up, especially in the first year after surgery when the band is being “tightened”. If you live several hours from your surgery center this can be difficult. Filling the band involves sticking the patient with a needle, so if you “hate shots,” a band may not be the right choice.
Band patients do not suffer adverse effects from eating sugars (dumping syndrome) so they need to be more disciplined in their food choices. Things like sodas, ice cream, cakes and cookies slide through the band easily, but obviously these choices will not lead to the desired goal of significant weight-loss.
Although the band has an excellent safety profile, there are complications that can occur with any weight-loss operation, and the band is no different. About 10 percent of patients will require a second operation to address a problem with their band.
Conclusion
Adjustable gastric banding is a safe, effective weight-loss operation that can lead to meaningful, sustained weight-loss. No matter what weight-loss operation is chosen, however, to ultimately be successful one needs to change their lifestyle and learn to work with the surgery.
Biliopancreatic Diversion with Duodenal Switch
By Debra Salvatore, RN, BS, CNOR, CFN
|
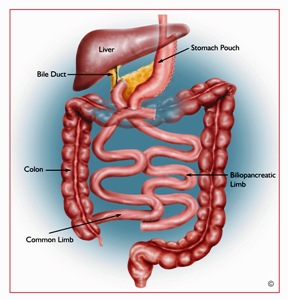
Gastrointestinal Tract after Biliopancreatic Diversion with Duodenal Switch |
 |
| ©2003-2006 Endo-Surgery, Inc. All rights reserved. Used by permission |
The Biliopancreatic Diversion with Duodenal Switch (BPD/DS) is most often an open operative procedure. It is performed in some bariatric centers laparoscopically, though in most cases, is still done “open.”
BPD/DS is based on a smaller stomach and combines a lower restriction and a high level of malabsorption. The outer margin of the stomach is removed (approximately two thirds), and the intestines are then rearranged so that the area where the food mixes with the digestive juices is short. A portion of the stomach is then left with the pylorus still attached and the duodenum beginning at its end. The duodenum is then divided, allowing for the pancreatic and bile drainage to be bypassed. It is a pyloric saving procedure, which eliminates the “dumping syndrome” that is inherent to gastric bypass.
The BPD/DS requires a much longer recovery period (usually six to eight weeks), causes the greatest risk for infection (due to the size of the incision, increased operative time and exposure of the digestive organs) and usually carries a 25 percent chance for development of incisional hernia post-operatively (due again to the length of the incision). The BPD/DS also carries the highest risk of nutritional deficiencies post-operatively due to malabsorption.
There are minimal iron deficiencies and B-12 deficiencies are not created by the Duodenal Switch. Of course, all patients are monitored for iron and B-12 as well as other water soluble vitamin deficiencies. Patients who undergo BPD/DS are able to enjoy nutritional foods and eat more normally without the restriction of a small pouch (one to two ounces) as in a gastric bypass.
The BPD/DS is a more invasive operation. According to a recent analysis, BPD/DS carries a mortality rate of 1.1 percent within 30 days after surgery.
The procedure allows for increased malabsorption, resulting in increased weight-loss. Foods high in fat content are not easily absorbed and will be eliminated along with the usually high calories associated with the high fat. In all weight-loss surgery options, carbohydrates and sugars are absorbed, so eating foods high in sugar (and calories) will still cause unwanted weight gain or inability to lose weight. In all weight-loss surgery options, emphasis is placed on nutritionally beneficial and nutrient dense foods.
BPD/DS patients enjoy “normal” sized food portions at meals. The BPD/DS allows patients to increase portion size over time, allowing for greater diversity in food consumption at each meal.
Patients are always encouraged to maintain the commitment to lifestyle and food changes associated with weight-loss. BPD/DS patients are asked to first increase protein intake, then vegetables, and lastly, if able at all, breads, pastas or rice in very limited amounts.
Editor’s Note: The Cover Story of this issue is designed to inform you of the various weight-loss surgery treatment options available. It is important to note that there are risks involved with bariatric surgery, as well as any other surgical procedure. Before making a treatment decision, it is important to discuss these risks with your physician and/or surgeon. The OAC also encourages patients to discuss these risks with their family members. For more information on the risks of bariatric surgery, click here.
About the Authors:
Robin Blackstone, MD, FACS, is a practicing bariatric sur-geon from Scottsdale, Arizona. Dr. Blackstone established the Scottsdale Bariatric Center. She is also the Vice Chairman of the Surgical Review Corporation, Center Review Committee. Dr. Blackstone is a member of the OAC Board of Directors.
Melissa Davis, RN, MSN, APRN,BC, NP-C, CNS, is a nurse practitioner, clinical nurse specialist, and registered nurse first assistant at the Scottsdale Bariatric Center, Scottsdale Arizona.
Lloyd Stegemann, MD, is a private practice bariatric sur-geon with New Dimensions Weight Loss Surgery/Weight Wise in San Antonio, TX. He was the driving force behind the Texas Weight-Loss Surgery Treatment Options Introduction Weight Loss Surgery Summit and in the formation of the Texas Association of Bariatric Surgeons (TABS) where he currently serves as President. He has been very active in the Texas state legislature trying to increase patient access to weight-loss sur-gery. Dr. Stegemann is a member of the American Society of Bariatric Surgery (ASBS) and the OAC Advisory Board.
Debra Salvatore, RN, BS, CNOR, CFN, is the Director of Bari-atric Services at North Oakland Medical Centers in Pontiac, Michigan. She continues to work in both fields of nursing. She was the Surgical Education Coordinator for six years at NOMC prior to becoming an administrator. She is a member of the OAC Advisory Board.
by Kendall Griffey, OAC Communications Manager Spring 2024 We have officially kicked off Your Weight Matters Regional…
Read Articleby OAC Staff Members Kendall Griffey and Michelle “Shelly” Vicari Winter 2024 In a world that often…
Read Articleby Rachel Engelhart, RD; Kelly Donahue, PhD; and Renu Mansukhani, MD Summer 2023 Welcome to the first…
Read Article









