Obesity and Asthma: How are they Related?

by Sunil Dainel, MD, FTOS
Fall 2017
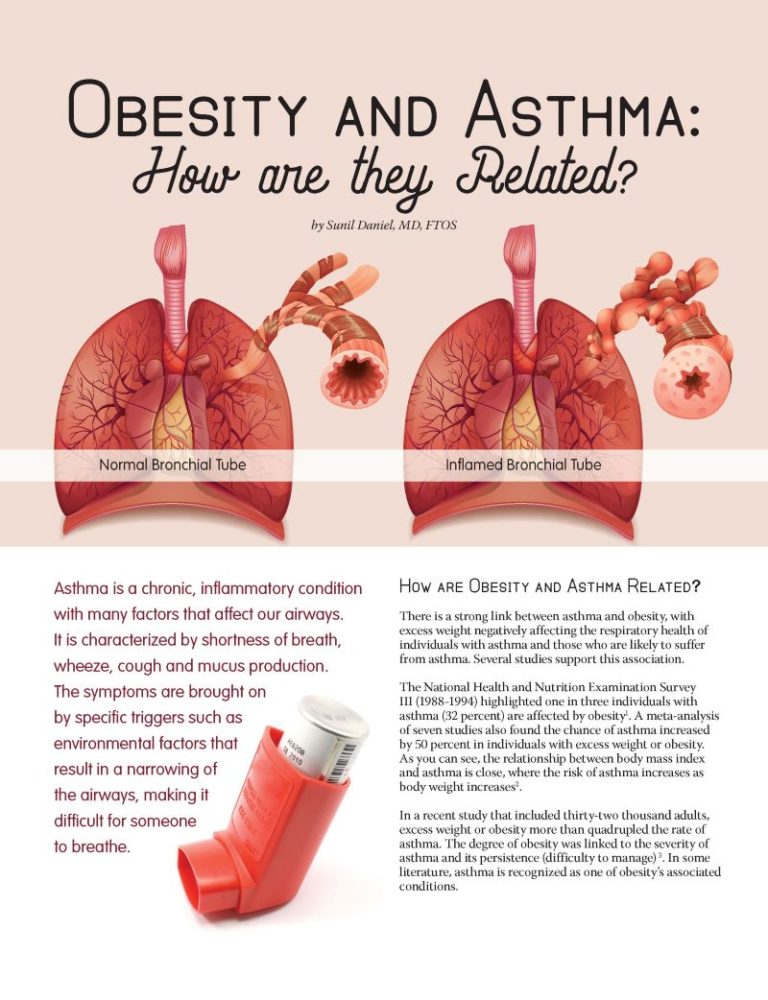
Asthma is a chronic, inflammatory condition with many factors that affect our airways. It is characterized by shortness of breath, wheeze, cough and mucus production. The symptoms are brought on by specific triggers such as environmental factors that result in a narrowing of the airways, making it difficult for someone to breathe.
How are Obesity and Asthma Related?
There is a strong link between asthma and obesity, with excess weight negatively affecting the respiratory health of individuals with asthma and those who are likely to suffer from asthma. Several studies support this association.
The National Health and Nutrition Examination Survey III (1988-1994) highlighted one in three individuals with asthma (32 percent) are affected by obesity1. A meta-analysis of seven studies also found the chance of asthma increased by 50 percent in individuals with excess weight or obesity. As you can see, the relationship between body mass index and asthma is close, where the risk of asthma increases as body weight increases2.
In a recent study that included thirty-two thousand adults, excess weight or obesity more than quadrupled the rate of asthma. The degree of obesity was linked to the severity of asthma and its persistence (difficulty to manage) 3. In some literature, asthma is recognized as one of obesity’s associated conditions. While we do not fully understand the exact process linking obesity and asthma,, there are some possible theories that have been proposed.
MECHANICS:
Obesity has a negative effect on lung volumes. Tidal volume is the amount of air that enters the lung at the end of inspiration (breathing in) and leaves the lung during expiration (breathing out). Functional residual capacity is the amount of air that remains in the lungs at the end of expiration, maintaining the lung volumes by keeping the small airways open. Having excess weight in the chest wall (making it difficult to expand outward) and abdominal area (pushing up the diaphragm, or the muscle below your lungs), decreases overall lung compliance and makes it difficult for them to expand, thus reducing tidal volume and functional residual capacity.
INFLAMMATION:
Obesity is considered a state of low-grade inflammation. This is caused by excess adipose tissue (fat cells) that release proteins such as interleukin-6 (IL-6) and Tumor necrosis factor-alpha (TNF-α) which increases inflammation. Leptin is a hormone secreted from fat cells. This hormone has an influence on energy levels by increasing the metabolism and food intake by decreasing hunger. Leptin also stimulates a specific type of immune cells, T-cells, to multiply and increase the production of pro-inflammatory proteins. It has been suggested that this increased inflammation can impact the airways of individuals with obesity. Some studies have been able to show an increase in neutrophils, a type of white blood cells, in the airways of individuals with obesity and asthma.
Can your Diet Affect your Asthma?
Diet is a common link between obesity and asthma. Obesity is recognized as a state of excess energy intake due to poor diet quality. Diet quality has an effect on the immune system causing airway inflammation, asthma exacerbation and its management. Fat is one of the major diet compositions. The amount and type of fat in the diet influences airway inflammation.
One randomized clinical study showed activation of the immune system and increased mucus four hours after consuming a high-calorie, high-fat meal. The increase in mucus was significantly higher in diets rich with trans-fat compared to those without. The quality of fat in the diet has a different effect on airway inflammation. The study also showed a decreased response to asthma treatment (bronchodilators) after high-fat meal consumption, highlighting the role of diet quality on asthma management.
Fruits and vegetables are high in fiber and low in energy density. Consuming these foods helps reduce calorie intake and boost weight-loss. In fact, studies have shown that 5-10 percent weight-loss leads to improvement in asthma control and quality of life in asthma patients. Fruits and vegetables are also high in carotenoids. Carotenoids are highly pigmented fat soluble compounds that are naturally present in fruits and vegetables, and also have an anti-oxidant (anti-inflammatory) property.
One clinical study randomized participants with asthma to a high-antioxidant diet (five servings of vegetables and two servings of fruit daily) or a low anti-oxidant diet (two or less servings of vegetables and one serving of fruit daily). Participants randomized to low anti-oxidant diets were two times more likely to experience asthma exacerbation and worsening of lung functions. This study showed that carotenoid supplements did not have the same effect on respiratory inflammation as consuming carotenoid through whole fruits and vegetables. This emphasizes the importance of not substituting supplements for fruits and vegetable intake5.
Can Physical Activity Help Improve Your Asthma?
Physical activity is important in weight management and weight maintenance. Other benefits of physical activity include improvement in:
- Cardiovascular disease
- Type-2 diabetes
- Hypertension
- And Inflammation, among others
Most individuals with asthma experience worsening symptoms after exercise (exercise-induced bronchoconstriction) which causes them to avoid physical activity. This can include weight gain, inflammation and decreased fitness levels. Exercise training is important for individuals with asthma. Exercise training is defined as training for 7 days per week, more than two times per week. Five or more training sessions per week have been shown to improve quality of life by 17 percent, lung volume (FEV1) by 3 percent and decrease airway sensitivity by 53 percent 6.
In a study of 46 Australian females who are affected by obesity and asthma, an exercise routine of one hour per week consisted of:
- Group personal training
- Attending gym three times a week
- Increasing steps per day to goal of 10,000 steps per day
This training resulted in a 50 percent reduction in sputum eosinophils (type of white cells)7. This highlights the role of increased physical activity on reducing airway inflammation. Even though weight-loss can be achieved through dietary restriction, it’s important to add physical activity. The benefits of dietary restriction and physical activity are:
- Decreases airway inflammation
- Improved lung function
- Better asthma control and quality of life
Conclusion:
While there is still more research to be done, there appears to be a link between obesity and asthma. If you are affected by asthma, it’s important to consider all of the factors that may be at play (such as having excess weight, consuming a lower-quality diet or not getting adequate physical activity). It is also recommended that you talk to your doctor about ways to improve your asthma and/or the potential conditions associated with it. Reducing your risk for asthma and improving its symptoms will likely help you achieve a higher quality of life and feel your best!
About the Author:
Sunil Daniel, MD, FTOS, is a board certified obesity medicine physician with fellowship training in clinical nutrition and obesity management. He is a fellow of The Obesity Society and has authored several scientific papers on obesity and its medical management. He also serves on the OAC Education Committee.
by Sarah Muntel, RD Spring 2024 Spring has sprung, bringing sunnier and warmer days! For many, this…
Read Articleby Yelena Kibasova Spring 2024 The fitness world is evolving, with new trends and innovations that promise…
Read Articleby Kendall Griffey, OAC Communications Manager Spring 2024 We have officially kicked off Your Weight Matters Regional…
Read Article









