Lipedema and Obesity


by Karen Herbst, PhD, MD
Spring 2014

Editor’s Note: The Lipedema and Obesity article featured a special patient perspective sidebar, Living with Lipedeman, written by Sarah Bramblette. To view this article, please click here.
What’s the Link?
Lipedema is thought to affect at least 11 percent or more of the female population in the U.S. and elsewhere, which translates to more than 16 million women in the U.S. alone that may have lipedema and not know it.
Why Can’t I Lose Weight in My Legs?
Female, or gynoid, fat under the navel, on the buttocks, hips, and thighs gives women their attractive curves. Gynoid fat increases during puberty and is smooth and soft in texture. But not all gynoid fat is the same. For example, what if you could not lose gynoid fat with strict eating and an intensive exercise regimen and instead, the fat continued to grow no matter what lifestyle changes you tried. What if the gynoid fat was painful, felt like heavy weights, and you bruised easily? This type of fat is called “lipedema,” meaning fluid in the fat, and is well-known to remain unresponsive to lifestyle changes.
Lipedema was first reported in the literature by Drs. Allen and Hines at the Mayo clinic in 1940. Since that time, knowledge in the area of lipedema spread across Europe, especially in Germany and Austria, and is now slowly advancing in the U.S., albeit 74 years after the initial published description.
As an example of recent progress, an application to the U.S. National Library of Medicine (NLM) was accepted and lipedema received a Medical Subject Heading (MeSH) code meaning that the term “lipedema” is now part of a comprehensive and controlled vocabulary that will facilitate searches for articles on lipedema in the NLM free database, PubMed, and confirms lipedema as a valid evidence-based entity. An application for an International Classification of Disease (ICD) code has also been submitted. The ICD code will allow healthcare providers who see and treat patients with lipedema to document clinical visits with a recognized code, which can pave the way for research, including prevalence studies to determine how common lipedema is amongst various groups, and will allow billing and payment through insurance providers.
What is Lipedema?
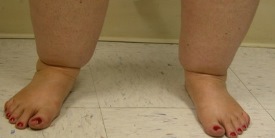
Lipedema is generally described as a symmetric and circumferential increase in fat of the buttocks, hips and legs, affecting the arms in most, sparing the upper abdomen, trunk, feet and hands. A cuff of fat can be present on the wrist or ankles where the lipedema fat ends and normal fat begins (Figure 1).
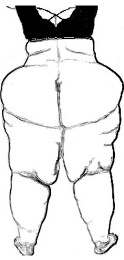
In later stages, lipedema fat can spread to the rest of the body. The lipedema fat itself is not smooth but feels like gelatin with small pea-sized nodules like foam balls in a bag. The excess fat growth on the buttocks, hips and legs gives a distorted pear shape to the body where the lower body is clearly out of proportion to the upper body (Figure 2). Healthcare providers have not had ample opportunity to be educated on the texture of normal fat; therefore, it is usually a physical or occupational therapist with experience in manual lymph drainage or a compression garment fitter who may notice the lipedema fat tissue and mention it to the patient. Many women find information on lipedema by searching the Internet for “painful fat legs.” Both mothers and fathers can pass lipedema to their daughters and various groups are currently searching for the genetic information that allows this to happen.
What is Going on under the Skin in Lipedema?
Normal fat cells are organized into groups called “fat lobules” that slide past one another under the skin along thin fibrils, so fat feels soft and smooth when the skin is pressed down. Investigators in Europe hypothesize that lipedema results from the accumulation of fat cells that have become very large in size (hypertrophied). These large fat cells stimulate production and recruitment of a molecule that can be several thousands of sugars (carbohydrates) long called “hyaluronic acid.” This long sugar structure is found naturally in all living organisms and binds water. The increase in hyaluronic acid and water gives the lipedema fat a stiff quality similar to gelatin, and the legs begin to feel heavy. The fat lobules that normally slide past each other on thin fibrils round-up in their geloid environment.
Hyaluronic acid and other molecules attract inflammatory white blood cells to the fat that produce damaging substances that injure the fat lobules, blood and lymphatic vessels, and other structures. As a result, the blood vessels break easily causing bruising. The lymphatic vessels, which initially pump more frequently in lipedema, start to fail and can swell. This process can eventually lead to the lymphatic vessels leaking, which allows more water to collect around the fat cells – causing the lipedema tissue to become heavy.
The body tries to repair, filling in inflamed areas with a scar around the outside of the rounded fat lobules allowing them to be felt as small beads through the skin. The pain of lipedema most likely results from nerves being damaged in the tissue as well as pressure on the nerves from excess trapped water.
Development of Lipedema
Lipedema fat develops in stages, though many women stay within stage 1 or 2 and do not progress to stage 3.
Stage 1
In Stage 1, the skin looks normal, but the amount of lipedema fat is increased.
Stage 2
In stage 2, there are indentations of the skin and underlying fat similar to a mattress. The fat contains larger mounds of fat that can be lipomas or in some cases, lipomas filled with blood vessels called angiolipomas.
Stage 3
In stage 3, bulky extrusions of skin and fat cause large deformations especially on the thighs and around the knees (Figure 2 ). Lymphedema, where lymph fluid leaks from lymphatic vessels, can develop during stage 2 or 3 lipedema, called lipo-lymphedema. Lipedema therefore is a pre-lymphedema condition, although not everyone with lipedema will develop lymphedema.
Lipedema is often confused with lymphedema but there are clear differences. Lymphedema results from a failure to pump lymph fluid out of the limb (in lipedema, lymph pumping can be slowed but not stopped) or damaged lymphatic vessels that leak an abundance of lymph fluid resulting in pooling in the hand or foot, eventually spreading up the arm or leg, respectively.
When one pinches the skin of the foot, a large hump of fluid-rich tissue is found in lymphedema (Stemmer’s sign positive) but in lipedema, the skin does not have fluid in it and can be easily lifted from the underlying fat tissue (Stemmer’s sign negative). Lymphedema often affects only one arm or leg whereas lipedema is symmetric.
Lipedema spares the hands and feet until later stages when lymphedema may occur, therefore the lymphedema that occurs with lipedema is a secondary condition rather than a primary lymphedema.
Lipedema is confused most times with lifestyle-induced obesity, which can create problems for the patient with lipedema as they and their providers become frustrated with their inability to lose the lipedema fat.
How Can Lipedema Fat be Managed?
The question of, “Why lipedema fat is hard to lose with lifestyle changes while non-lipedema fat can be lost?” remains unanswered. One theory is that size of the fat cells and the geloid layer of hyaluronic acid and water move the fat cells farther away from blood vessels and therefore slow the release of fat. The sheer number of fat cells in the gynoid area is much higher in women than men, just as the number of fat cells in the abdomen is higher in men than in women. The fat cell load in the gynoid area in women compared to the hands, feet and trunk equates to more fat needed to lose. Inhibiting the release of fat molecules from fat cells can make fat cells very large. Further research into this area may help explain the origin of large fat cells in lipedema.
Treatment of lipedema is focused primarily on decreasing fluid in the tissue by:
- manual lymph drainage therapists who gently open lymphatic channels and move the lymphatic fluid using hands-on techniques
- exercise including whole body vibration and swimming, exercises that have been proven to move lymphatic fluid
- some supplements and medications that help with lymphatic pumping
- compression garments that keep the fluid at bay and assist the sluggish lymphatic flow
Anecdotally, patients have not shown loss of lipedemic fat after extreme caloric restrictive diets. However, healthy eating is very important for people with lipedema as the growth of normal fat is thought to promote lipedema fat growth. Lymph sparing tumescent liposuction and water jet assisted liposuction are the only methods that are known to reduce the number of lipedema fat cells at this time. Having refined these techniques throughout the last 20 years, many German surgeons are proficient and actively training surgeons in the U.S. in liposuction methods specific for lipedema fat. Research into resolving lipedema in the absence of surgical measures is needed.
Evolution and Lipedema
Why would so many women have lipedema fat? Gynoid fat is well known to be healthy fat that protects against heart disease. Gynoid and lipedema fat take up fat and sugar from the blood and lymphatic vessels after meals quickly and efficiently so that blood vessels remain clean of fatty plaque and the risk for diabetes remains low. The development of large fat cells and hyaluronic acid in people with lipedema and or diabetes may serve a protective function to reduce blood fats and sugars. Lipedema fat is however dangerous when it progresses onto the abdomen and trunk especially resulting in a risk or development of high blood pressure, high cholesterol, and diabetes. Lipedema fat is therefore not benign or simply a cosmetic nuisance, but deserves serious study and development of interventions.
Doctor’s Box
As an Endocrinologist that helps patients manage weight, I see many women interested in surgical weight-loss who have undiagnosed lipedema. Women with lipedema who want to and are eligible to undergo bariatric surgery, in addition to maintaining a healthy diet and exercise, must be under the care of a manual lymph drainage therapist before and after the surgery to avoid failure of the procedure to promote weight-loss, and risk of development of lymphedema.
Summary
Lipedema is a condition of excess gynoid fat that while cardio-protective early-on, can result in deformations of the body, disability and development of diabetes. The underlying pathophysiology of large fat cells and surrounding hyaluronic acid and water can also be found in diabetes, therefore studying the fat in either condition is crucial. Current treatment of lipedema includes liposuction of the fat cells, healthy diet and exercise, and manual treatments to keep the fluid to a minimum. More research is needed in the area of lipedema to help the millions of women affected by this condition.
About the Author:
Karen Herbst, PhD, MD, is an Associate Professor at the University of Arizona where she practices Clinical Endocrinology and sees patients with fat disorders. She is a board member of the Fat Disorders Research Society whose goal is to educate the public and healthcare providers about fat disorders.






