Beyond the Looking Glass: An Honest View of Body Dysmorphic Disorder


by Merrill Littleberry, LCSW, LCDC, CCM, ACE-CPT
Summer 2019
I’m too tall, I’m too short,
my hair is too curly,
my hair is too straight,
I’m too pale, I’m too dark ……
Let’s be honest. We all have at least one thing we wish was different about our appearance. If you have occasional thoughts about the size of your thighs or how large your hips are, you do NOT have a disorder. Trying to look your best by using extra makeup, a push-up bra or some Spanx does NOT qualify as a disorder. Even if you’re a person who appears to be overly set on losing that extra 10 pounds or ridding yourself of cellulite, you do NOT meet the criteria for an official medical diagnosis.
However, it is another story if the previous examples become:
- Uncontrollable, constant negative thoughts
- Extreme sources of stress in your life
- Repetitive unstoppable behaviors
- Overtakes hours of your day
Then YES, you should see a healthcare professional to address them.
What is Body Dysmorphic Disorder?
Body dysmorphic disorder (BDD) is very different from being unhappy with how you look on a bad day. It is far beyond the everyday complaints about hair or weight most people have. BDD is a debilitating, time-consuming, ritual following, psychiatric diagnosis. It is an obsessive disorder that forces a person to focus all of their thoughts on a personal flaw—real or imagined. This is not a disorder to be ignored or minimized. It can be an emotionally damaging way of thinking that negatively impacts every part of someone’s life.
Putting it into Perspective
We have all stared into a mirror under terrible lighting and magnification, only to see how imperfect we actually are. That stray hair suddenly looks like a tree trunk growing from your chin and becomes the center of your attention. We seem to have a natural habit of looking for, and focusing on, the smallest flaws we can find. We then try to find a way to fix, live with or ignore the newly found flaw. We may pluck it, tuck it or bleach it. We can even razor, laser or wax it. After that we tend to go on with our daily routine, giving it little to no thought.
Entire industries succeed on our desire to look our best. Procedures to look more like flawless celebrities are created daily. Thousands of dollars are spent by everyday people wanting to be the perfect image they see in magazines and on television.
The idea of looking perfect fills our brains at every stage of life. However, nearly everyone looking to spend money and have procedures done still does NOT qualify as having BDD.
The Reality of Body Dysmorphic Disorder
BDD consumes a bit of every minute, of every hour, of every day. It can steal three to eight hours of a person’s day. It fills their brains with negative and damaging thoughts. Think about it this way: a 15-year-old who develops BDD will lose two to five years of their life by their 30th birthday obsessing over how they look.
Understanding Body Dysmorphic Disorder
To better understand BDD, think about obsessive-compulsive disorder, also known as OCD. Most of us have a basic understanding of OCD. We can think of somebody who may be obsessed with germs. This person cannot stop the thoughts in their mind about germs and coming in contact with them. These thoughts negatively impact the activities of daily life due to repeated hand washing and cleaning surfaces.
BDD is in the family of obsessive-compulsive disorders. Healthcare providers use a reference guide called the Diagnostic Statistical Manual (DSM-V). In today’s edition, under obsessive-compulsive and related disorders, five primary conditions are listed.
Three of the five are:
- Hoarding
- Trichotillomania (the pulling of hair)
- Excoriation (the picking of skin)
To understand BDD, you need to know that this disease causes someone to have never-ending thoughts and a laser-like focus on how they look. These thoughts can be centered on their whole body, a specific part of their body or a real (or imagined) flaw. In rare cases of BDD, the focus is on body odor.
Understanding Body Dysmorphic Disorder In-depth
The flaws a person with BDD sees—real or imagined—cannot usually be seen by others and generally would not bother someone without BDD. Yet, for someone with BDD, it is as if a neon arrow is pointing out the flaw to the world. These suffocating thoughts result in repetitive behaviors which cause so much distress that they keep someone from daily life. An example might be a person who wishes to only be alone, drops out of school or is afraid to meet new people. This can seem to mirror social anxiety. However, if someone is only choosing these behaviors because of how they feel others see them and their “flaws,” it is classified as BDD.
BDD is not an eating disorder, even when someone’s believed flaws center around body fat or weight. BDD can only be diagnosed when it is known that the individual does not have an eating disorder.
BDD often results in extreme, repetitive behaviors such as excessive grooming, compliment seeking or the ongoing need for reassurance of how they look. This disorder also causes the person emotional pain from constantly comparing themselves to others.
Adolescents and young adults that suffer from BDD often find it hard to cope with their symptoms while at a traditional high school or college. Studies have found this leads to an increase in suicide attempts and a high school drop-out rate of 20% among sufferers of BDD.
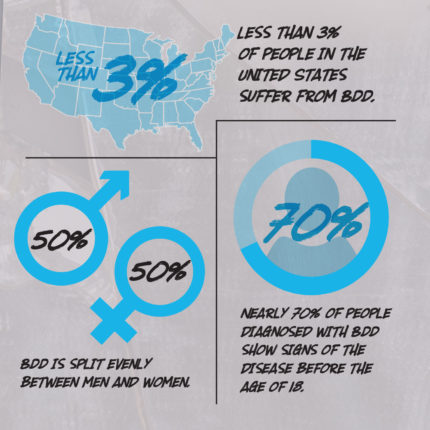
How Common is BodyDysmorphic Disorder?
What Causes Body Dysmorphic Disorder and is it Treatable?
Where does it come from and how do we get it? BDD most often occurs in victims of childhood neglect or abuse. It can also be seen more when an immediate relative has a form of OCD.
The refreshing news is that BDD is treatable. Beneficial treatment options usually include behavioral therapy combined with medication.
A patient once said to me, “When I started treatment it felt like a boomerang. The minute I get rid of it, it comes soaring back. Now it takes much longer for the boomerang to loop back around and I am ready for it.” She is a wonderful work in progress!
If you suffer from the thoughts discussed above, I suggest you seek out resources explaining these disorders. Visit iocdf.org for resources and information you can use to learn more.
Conclusion
There are enough people in the world who will dislike you simply because of your appearance. They will dislike you before they ever get to know you. People will look for your flaws and weaknesses no matter your size or color. My one suggestion to you is this: don’t be one of those people. Learn to love the you you’re with.
About the Author:
Merrill Littleberry, LCSW, LCDC, CCM, ACE-CPT, is a healthcare professional in the field of mental and physical health. She believes mental and physical health are equally important, stating one cannot function optimally without the other. She is known as “Vitamin M,” a motivational speaker, psychotherapist and personal trainer along with many other roles. She hopes the role she will be remembered by is a dedicated advocate who continually discovered ways to improve the lives of others.
by Sarah Muntel, RD Spring 2024 Spring has sprung, bringing sunnier and warmer days! For many, this…
Read Articleby Robyn Pashby, PhD Winter 2024 “No one is ever going to date you if you don’t…
Read Articleby Leslie M. Golden, MD, MPH, ABOM Diplomate Winter 2024 The journey to overcoming obesity is a…
Read Article