“Band over Bypass”

by Helmuth T. Billy, MD
Summer 2012
After the announcement that singer Carnie Wilson had undergone the “band over bypass” procedure in January 2012, a lot of attention has been directed at the operation and what kind of patient would be appropriate to consider “band over bypass.” The proper selection of potential patients and establishment of expectations is essential if an individual is going to have any level of success with this procedure.
Gastric bypass surgery may still be the most reliable and predictable bariatric operation available when it comes to significant weight-loss, treatment of type 2 diabetes, hypertension and sleep apnea. Individuals undergoing this procedure are amazed at the ease with which their weight drops and health improves. With a stomach little bigger than the size of a thumb, it seems almost impossible that anyone could regain any of the weight that the gastric bypass helped them lose.
Unfortunately, sometimes years after a successful gastric bypass, as they see the scale increasing, some post-surgery patients are left wondering, “Why isn’t my surgery working anymore?” Even the most successful gastric bypass patients have seen their body mass index (BMI), once again, reach the point where they become affected by severe obesity.
Weight Regain
Obesity is a chronic, relapsing disease and long-term success is intimately linked to long-term changes in behavior. In many post-surgery patients, even subtle behaviors, which if they return, can lead to eating habits that overpower even the most successful gastric bypass operation. This can lead to weight regain and feelings of disappointment and frustration. Some individuals who experience weight gain following gastric bypass have not been seen by a bariatric surgeon for years following their operation. If weight regain comes full circle, surgeons performing gastric bypass surgery have only a few options to try to get their patients “back on track.”
“Band over Bypass”
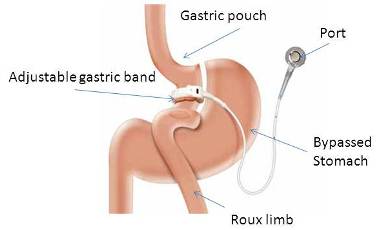
“Band over bypass” (pictured right) refers to one of the tools surgeons have available to assist patients who gained weight after what was initially a successful gastric bypass operation. The concept is fairly simple. If after a thorough evaluation, a patient who experienced significant weight regain and who has already undergone gastric bypass might have the option of placing a laparoscopic adjustable gastric band (LAGB) to assist them in feeling fuller and eating less.
Weight regain after gastric bypass surgery is a fear every individual has tucked away in the back of their mind. If weight regain occurs, there are only a few options physicians have available:
- Do nothing more surgically – focus on diet, exercise and behavior.
- Evaluate the patient for a possible second gastric bypass or other stapled bariatric operation.
- Evaluate the patient for possible placement of a LAGB.
Re-doing Gastric Bypass and Safety
Initially, our focus as physicians centers on diet, exercise and behavioral changes. When these changes do not help, surgeons start examining the gastric bypass more closely. Patients often ask, “Did my pouch stretch?” and in some cases, surgeons can identify large stomachs which could be made smaller by “re-doing” the gastric bypass. Unfortunately, doing a gastric bypass a second time, stapling, trimming the stomach down to a thumb-sized stomach and redoing the connection between the stomach and the small intestine is a high-risk procedure, one that many surgeons would rather avoid.
Re-doing a gastric bypass a second time also does not address the reason why the patient regained weight, basically poor eating and exercise behaviors that may have eroded away what was once a successful operation. Because of the risks involved with attempting a second gastric bypass, many surgeons and patients began looking at a safer alternative.
Four Essential Behaviors that Improve the Ability of Bariatric Patients to Decrease Calorie Consumption and Enhance Weight Maintenance.
- Drink water. Consumption of drinks with artificial sweeteners can stimulate hunger and lead to snacking. It is actually not that difficult if each day my patients have a goal to drink water instead of diet drinks or those with artificial sweeteners. Drinking water is never a mistake.
- Don’t eat with your fingers. If you think about all the things we eat using our fingers, almost all of them are foods we should avoid. Snack foods, chips, candy, crackers, cookies, string cheese and breads are all foods that we mindlessly access. Vegetables are the ONLY exception. My patients can snack on all the vegetables they want, just don’t dip them in ranch dressing. The concept of avoiding eating with your fingers will eliminate eating in your car, in front of the television, at the movie theater or standing in your kitchen.
- Stay out of fast food restaurants. Make your own lunch. When you take the time to make your own lunch, you pay more attention to the types of foods you are packing to eat.
- Start exercising. Start taking a 10 minute walk every day. The key here is every day. Almost everyone has time for a 10 minute walk outside. Doing this every day is easy to accomplish and starts the process of establishing an exercise program. Do not mislead yourself with the answer, “I don’t have time.”
Candidates for “Band over Bypass”
“Band over bypass” is simply placing a LAGB in a patient who has already undergone a gastric bypass. A LAGB is an inflatable ring placed around the very top of the stomach to help create fullness and satisfaction when eating. It is adjustable and the tightness of the band can be set at different levels for the specific needs of each patient. Placing a LAGB on a patient who has already undergone a gastric bypass is considered a revision operation and as such, a complete evaluation is essential before any surgery is performed.
In our practice, patients who were initially successful with their gastric bypass, but throughout the course of five to 10 years experienced significant weight regain, can undergo evaluation to see if they are appropriate candidates to consider “band over bypass.” The evaluation includes endoscopic examination of the gastric bypass, radiology studies to see what the gastric bypass looks like and if it is the proper size to consider placing a LAGB.
In addition, it is important to identify the eating and lifestyle behaviors which led to weight regain. We spend considerable time with dietary consultations and behavior analysis, including psychological assessment, as they are important in evaluating each patient in order to focus on the behaviors and lifestyles which led to weight regain. Even patients who state that, “I’m eating healthy,” or “I think I’m eating too much,” usually overlook simple behaviors which lead to mindless eating and excessive calories.
The ideal patient to consider for “band over bypass” has a small gastric pouch, one that was not dilated from chronic overeating and has identifiable eating habits and behaviors that led to weight regain.
Benefits of “Band over Bypass”
“Band over bypass” has the benefit of focusing on combining a surgical approach with a behavioral focus to assist the patient in eating less while eliminating the habits and behaviors which can sabotage or damage an effective gastric bypass. The benefits of being able to place a LAGB rather than using staples or having a second attempt at gastric bypass is one of patient safety. It has been well established that the LAGB has an excellent safety record and is a relatively low-risk procedure when placed by experienced surgeons in credentialed facilities.
Importance of Pre-operative Evaluation
Pre-operative evaluation is important. If the gastric pouch created by gastric bypass is the right size and shape, then placing a LAGB on those patients can be as straightforward as placing a LAGB on an individual who has never had bariatric surgery.
One of the benefits of using a LAGB is that success with a LAGB is dependent on the patient returning regularly to their surgeon, focusing on eliminating behaviors which can cause overeating, snacking, grazing and poor food choices. Patients who are not committed to follow-up, lifestyle changes and behavioral changes tend not to do well with any revision surgery. Patients who are looking to “fix my gastric bypass” do not do well with “band over bypass.” Success for a patient considering placement of a LAGB over their gastric bypass is dependent on identifying those behaviors which can lead to weight regain and doing a surgical procedure which can enhance fullness, satiety and eating less.
Conclusion
After performing “band over bypass,” I expect the patient to come back to our office every four to six weeks for follow-up where our nursing staff, dietitian and psychologist can assist in solidifying post-operative behavioral changes which enhances the effectiveness of the procedure.
The LAGB procedure is a safer alternative to stapling or re-doing a gastric bypass, but it is not without its own set of risks. The device can erode into the gastric pouch requiring subsequent removal. The device can become infected or could move out of position requiring re-operation or removal. These risks are uncommon; however, it is important to consider all these risks before proceeding with any operation. “Band over bypass” is a revision operation and as such has risks that are different than those of people having bariatric surgery for the first time.
We have found “band over bypass” to be useful for assisting patients who gained significant weight following gastric bypass when combined with an intensive program of follow-up and implementation of new behaviors, such as those listed in this article. “Band over bypass” is not a new idea and results have been published in medical journals with varying degrees of success of the past few years.
Weight regain after gastric bypass happens to some of the most successful patients. Placing a LAGB over a gastric bypass can give back a feeling of restriction similar to what patients experience when their gastric bypass was new. This feeling of satiety can enhance a patient’s ability to limit their food intake. The LAGB can help control the outlet of the gastric bypass and by altering the tightness of the band, many patients can benefit from a feeling of restriction which was lost throughout time. In properly selected patients, we see improved ability for weight-loss and regain of the original effectiveness of their gastric bypass.
Insurance Coverage
We have had many of our patients have the placement of their LAGB procedure covered by their insurance, even though they have had a previous gastric bypass
operation. Insurance companies each have their own criteria regarding revision surgery and LAGB placement.
“Band over bypass” is considered a revision operation and as such, each insurance company might have specific criteria regarding how their plan members would qualify for this procedure or any other proposed revision operation. It is best to check with your respective health insurance company regarding benefits of coverage for revisional bariatric surgery before proceeding with any evaluation.
About the Author:
Helmuth T. Billy, MD, graduated from the University of California Berkeley and attended medical school at the University of California Davis. He has been in private practice since 1997 and performed his first LAP-BAND® procedure in September 2001, shortly after the LAP-BAND® was approved by the FDA. He currently practices in Ventura California and offers gastric bypass, sleeve gastrectomy, LAP-BAND® as well as revision of previous bariatric operations. He is a member of the American Society for Metabolic and Bariatric Surgery (ASMBS) and participates in the Centers of Excellence program.
by OAC Staff Members Kendall Griffey and Michelle “Shelly” Vicari Winter 2024 In a world that often…
Read Articleby Rachel Engelhart, RD; Kelly Donahue, PhD; and Renu Mansukhani, MD Summer 2023 Welcome to the first…
Read ArticlePost-operative addiction is often overly simplified as transfer addiction or cross-addiction, assuming individuals “trade” compulsive eating for…
View Video









