Current State of the Treatment of Obesity


by Stephen Boyce, MD
Fall 2014
Please Note: As of February 2020, the Food and Drug Administration has issued a voluntary withdrawal of Belviq, Belviq XR (lorcaserin) from the U.S. market, as a safety clinical trial has shown an increased occurrence of cancer. Patients currently taking Belviq have been advised to stop taking the medication and speak with their healthcare provider about its continued use.
Obesity continues to be a serious health concern claiming hundreds of thousands of lives worldwide annually. So much of our thinking around obesity, its pathophysiology (disordered physiological processes associated with disease or injury), and how surgical procedures actually work has changed throughout the past 10 years.
We know that obesity has all the hallmarks of a chronic disease and has been classified as a disease by a number of influential organizations, including the American Medical Association, other organizations, including the Obesity Action Coalition (OAC), The Obesity Society, the American Society for Metabolic and Bariatric Surgery, the World Health Organization, the Centers for Medicare/Medicaid Services, and the Social Security Administration to name a few.
Classifying Obesity
Like any other disease, the most appropriate treatment for obesity is dependent upon its severity. In medicine, we classify the severity of obesity based on a calculation called the body mass index (BMI).
Body Mass Index (BMI)
- A healthy weight individual is generally considered to have a BMI of 20-24.99.
- Medically, a person is “overweight” if their BMI is 25-29.99.
- A person suffering from obesity has a BMI of 30-34.99 and would be considered to have “severe obesity” if their BMI is greater than 35-39.99 in combination with a weight-related medical problem or a BMI more than 40 without any weight-related medical problems.
Severe obesity is sometimes called “morbid obesity” because that is when we start to see other diseases develop in patients as a direct result of the obesity. That is to say the obesity is causing our patients to have the morbidity of other diseases like diabetes, hypertension and sleep apnea. The term “morbid obesity” has, however, developed a negative/offensive connotation and the term “severe obesity” is preferred.
Metabolic Set Point
Throughout the past 10 years, much has been learned about the pathophysiology of obesity and the mechanisms by which surgery appears to work in patients suffering from severe obesity when nothing else has been effective in providing lasting weight-loss. The disease of obesity is multifactorial with genetic, environmental, and behavioral components. However, one of the predominant concepts that have emerged about the cause of obesity is that of the “metabolic set point” and thinking of bariatric surgery as “metabolic surgery.”
Through a series of elegant experiments at Harvard and the University of Cincinnati, Dr.’s Kaplan and Seeley (and others preceding them) have suggested that we all have a “metabolic set point” and that what our bodies defend is how much “energy” or fat our bodies store. If that is true, then to try to change the amount of fat we have would be fighting our bodies’ natural physiology. It would be like someone trying to eradicate his or her high blood pressure through sheer willpower.
This set point is probably programmed by our genetics and appears to be regulated by the secretion of hormones from our intestines, brain and adipose tissue. This knowledge is very liberating and hopefully will help dispel the negative connotations associated with patients suffering from obesity. Hopefully, it will also help people avoid the negative thoughts and self-deprecation that is all too often associated with their disease.
Treatment Options
Regarding treatment, if a person suffers from excess weight or obesity, the most appropriate treatment would include behavior modification (diet and exercise) and medical weight management. There are a few new medications for obesity that have been approved within the last couple years such as Qsymia® and Belviq®. The patient who suffers from severe obesity, however, is oftentimes treated with one of the surgical options, several of which have withstood the test of time and are approved by the Food and Drug Administration (FDA).
Non-surgical Treatment Options
This is the mainstay of treatment for people suffering from excess weight and obesity. The good news is that in addition to diet, exercise and our old friend phentermine, the FDA has approved two new drugs for our arsenal. The FDA also recently approved an additional obesity drug in September, Contrave® (naltrexone-bupropion).
Qsymia® is a combination drug (phentermine and topiramate ER) whose mechanism of action is not well understood. Clinical trials showed that the drug was safe and provided significant weight-loss. As a result, in 2012 the FDA approved the drug to be used as an adjunct with diet and exercise for chronic weight management in adults with a BMI of > 30 or as low as 27 with co-morbid conditions.
Belviq® (lorcaserin HCI) is a serotonergic drug that acts as an appetite suppressant. It was also approved by the FDA in 2012 for adults with a BMI of > 30 or as low as 27 with co-morbid conditions.
Surgical Treatment Options
Surgical treatment is the mainstay for the person suffering from severe obesity. We used to discuss the operations based on their presumed mechanism of action such as providing “restriction” or “malabsorption” for our patients. In light of our new understanding of the metabolic nature of the disease of obesity, we now are inclined to classify and talk about the different operations based on their ability to alter our metabolism.
The available approved operations vary our physiology (the way our bodies regulate energy storage levels) to differing degrees with some having no effect on physiology (non-metabolic operations) and others altering the physiology in a way that decreases our bodies’ desired storage level for energy or fat, suppresses appetite, and increases energy expenditure (metabolic operations).
Normally our appetite is controlled at least in part by the secretion of intestinal hormones, some of which make us feel hungry (orexigenic hormones) and some of which take our hunger away (anorexigenic hormones). The most commonly referenced orexigenic hormone is made by the stomach and is called ghrelin. Examples of well-studied anorexigenic hormones include GLP-1, PYY, CCK, and amylin.
Non-metabolic Operations
The options in this group provide significant weight-loss without altering the physiology of energy (fat) storage includes the laparoscopic adjustable gastric bands (LapBand® and the Realize Band®). They are considered non-metabolic options because they do not alter the body’s normal mechanisms that occur when dieting. With bandings and with dieting, orexigenic hormones increase and anorexigenic hormones decrease.
Metabolic Operations
The operations in this group help patients lose weight by altering their gastrointestinal tracts. Examples include the vertical sleeve gastrectomy (VSG), Roux-En-Y gastric bypass (RNYGB), and the biliopancreatic diversion with duodenal switch (BPD/DS).
Non-metabolic Operations
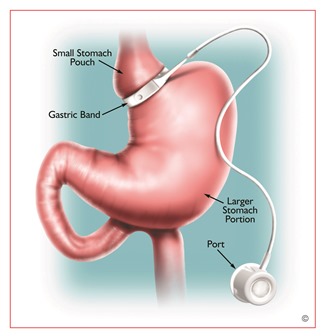
Laparoscopic Adjustable Gastric Bands
How they work:
The bandings provide significant weight-loss by restricting the amount of healthy food one can consume during a meal.
What is done:
The operation involves placing a silastic band around the upper part of the stomach. The band partitions the stomach into an upper small pouch and the rest of the body of the stomach below. The band’s job is to provide “restriction” to the flow of healthy food into the body of the stomach. Restriction is obtained by inflating the balloon inside the band with saline. This makes the band tighter on the stomach; therefore, slowing the passage of food from the upper pouch into the body of the stomach. Patients’ weight-loss is optimized if they receive four to six band “fills” in the first year after surgery.
Weight-loss:
Weight-loss is usually slow and steady with a goal of one to two pounds/week in the beginning. The bandings typically provide an excess weight-loss in the range of 35-50 percent for the typical patient throughout the long term. This amount of weight-loss usually leads to significant improvement in weight-related medical problems such as diabetes, hypertension, and obstructive sleep apnea.
Advantages:
Since the bandings do not alter the gastrointestinal tract, recovery is faster. The surgery is often safely accomplished as an outpatient or a 23-hour stay. Recovery is usually quick with most patients returning to work in about one week. The risk of death is very low with reported rates of 0.1 percent or less.
There is a low risk of developing nutritional deficiencies since the bowel is not rearranged in any way and, therefore, there are fewer vitamin and mineral supplements needed after surgery. The band is relatively easy to remove, thus restoring the gastrointestinal tract to normal.
Disadvantages:
The most commonly cited disadvantage is the overall lower amount of weight-loss by the average patient. The bands are associated with the highest rate of re-operation with 10-30 percent of the patients requiring band removal or conversion to another operation usually for failed weight-loss, band erosion, or band slip.
Metabolic Operations
How they work:
The approved operations in this class help patients have lasting significant weight-loss by altering the patient’s physiology in a way that lowers their metabolic set point for how much energy or fat their bodies naturally want to store. They also decrease appetite and increase energy expenditure. This is achieved by altering the gastrointestinal tract in a way that decreases orexigenic hormones and increases anorexigenic hormone secretion in response to food and weight-loss. These changes are accomplished by two means.
First, there is reduction in the hunger-producing hormone from the stomach (ghrelin) by either resecting or dividing the stomach in two.
Second, there is an increase in the satiety-producing hormones from the last part of the small bowel and pancreas (GLP-1, PYY, CCK, amylin). This is triggered by getting food to the last part of the small bowel faster through promoting faster transit or by bypassing part of the small bowel. This combination allows the patient to lose more weight with less appetite and hunger feelings.
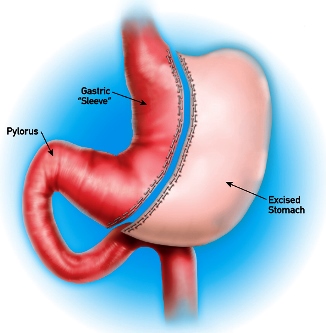
Vertical Sleeve Gastrectomy (VSG)
The VSG is a relative newcomer as a stand-alone weight-loss surgical procedure. Today, it is the most frequently performed bariatric operation. Medicare approved it in 2012 and most private insurers have followed. The VSG is performed by removing approximately 80 percent of the stomach. Almost all of the part of the stomach responsible for ghrelin production (the fundus of the stomach) is removed, which leads to decreased appetite and seems to influence the resolution of diabetes because ghrelin is diabetogenic (promotes diabetes). The remaining stomach is a tubular pouch that resembles a banana. The stomach may initially only have a capacity of 2 or 3 ounces. This smaller stomach reduces food capacity and empties faster than a normal sized stomach; therefore, food gets to the distal bowel quicker where the anorexigenic hormones are secreted.
Advantages:
It is a metabolic operation with weight-loss equal to a Roux-En-Y Gastric Bypass (RNYGB). Patients may expect to lose about 60-70 percent of their excess weight. However, patients with a BMI > 50 may not achieve the weight-loss they need with a sleeve alone. It is perceived as a simpler operation because there is no re-routing of the intestines. If the patient needs further weight-loss later, the VSG is easily converted into a biliopancreatic diversion with duodenal switch (BPD/DS).
Disadvantages:
The VSG is the only operation that is completely non-reversible. Life-long vitamin and mineral supplementation is required because, even though there is no bowel bypass, there are nutritional consequences of removing 80 percent of the stomach and absorption of vitamins and minerals are affected. Patients with a BMI > 50 may not lose enough weight with VSG alone. Because it is relatively new, we do not know what the risk of inadequate weight-loss or significant weight regain is (but in my opinion, will likely be similar to the risk after RNYGB).
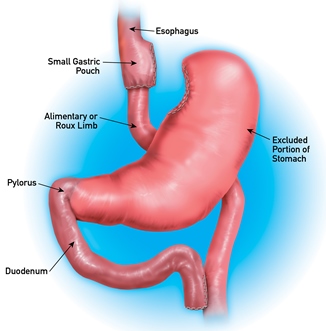
Roux-En-Y Gastric Bypass (RNYGB)
The RNYGB, until recently, was the most commonly-performed bariatric surgery worldwide. It has been around for almost 50 years and has been done laparoscopically since the early 1990’s.
There are two parts to the procedure. First, a small stomach pouch, approximately one ounce in volume, is created by dividing the top of the stomach from the rest of the stomach. Next, the small intestine is divided about one to two feet from the stomach (the average person has about 20 feet of small intestines), and the bottom end of the divided small intestine is brought up and connected to the newly created small stomach pouch.
The procedure is then completed by connecting the top portion of the divided small intestine back to the small intestine 3-5 feet further down so that the stomach acids and digestive enzymes from the bypassed stomach and first portion of small intestine will eventually mix with the food.
Similar to most bariatric procedures, the newly created stomach pouch is quite small and facilitates significantly smaller meals than normal. This translates into fewer calories consumed. Additionally, because there is less digestion of food by the smaller stomach pouch, and there is a segment of small intestine that would normally absorb calories as well as nutrients that no longer has food going through it, there is probably to some degree less absorption of calories and nutrients. Most importantly, the rerouting of the food stream produces changes in gut hormones that promote satiety, suppress hunger, and reverse one of the primary mechanisms by which obesity induces type 2 diabetes.
Advantages:
We have a great deal of experience with the RNYGB and know how to help patients with complications should they arise. It is a metabolic operation with all the benefits. The long term weight-loss (60-70 percent excess weight-loss) and resolution of co-morbid diseases is excellent. It is a great option for patients with severe gastro-esophageal reflux with a high rate of resolution of reflux symptoms.
Disadvantages:
There is an increased risk of ulcers with the RNYGB. The ulcers form in the small intestines next to the gastric pouch and are a source of bleeding, blockage and pain. Because smoking and NSAID’s (nonsteroidal anti-inflammatory drugs, like aspirin, ibuprofen, etc.) promote ulcers, these MUST be avoided after RNYGB. About 25 percent of patients will have inadequate weight-loss or weight regain long term after RNYGB. Like other metabolic operations, it is important to follow the recommended vitamin and mineral supplementation for the rest of your life.
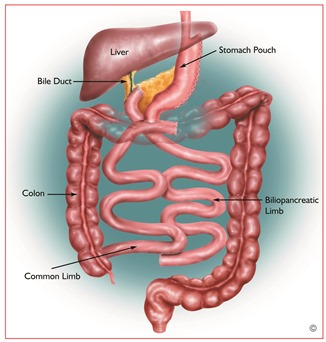
Biliopancreatic Diversion with Duodenal Switch (BPD/DS)
The duodenum, or the first portion of the small intestine, is divided just past the outlet of the stomach. The stomach is sleeved similar to but larger than (should hold about 6 ounces) a VSG. Then, an 8-9 foot long segment of the distal (last portion) small intestine is then brought up and connected to the outlet of the newly created stomach, so that when the patient eats, the food goes through a newly created tubular stomach and empties directly into the last segment of the small intestine. Roughly 60 percent of the small intestine is bypassed by the food stream. The bypassed small intestine, which carries the bile and pancreatic enzymes (the biliopancratic limb) that are necessary for the breakdown and absorption of protein and fat, is reconnected to the last portion of the small intestine so that they can eventually mix with the food stream.
Similar to the other surgeries described in this article, the BPD/DS initially helps to reduce the amount of food that is consumed; however, throughout time, this effect lessens and patients are able to eventually consume near “normal” amounts of food. Since the food does not mix with the bile and pancreatic enzymes until very far down the small intestine, there is a significant decrease in the absorption of calories and nutrients (particularly protein and fat) as well as vitamins dependent on fat for absorption (fat soluble vitamins). Lastly, the BPD/DS, similar to the RNYGB and VSG, affects gut hormones in a manner that impacts hunger and satiety as well as blood sugar control. The BPD/DS is considered to be the most effective surgery for the treatment of diabetes.
Advantages:
The BPD/DS provides the greatest weight-loss (often in excess of 80 percent excess weight-loss) and seems to be especially well-suited for our patients with a BMI of > 50. Co-morbid diseases like diabetes, high blood pressure and sleep apnea resolve to a greater extent with the BPD/DS than with any of the other operations. Fortunately, this operation also has the lowest risk of inadequate weight-loss or weight regain (<5 percent), which may be the most attractive feature of all.
Disadvantages:
There is a higher risk of serious malnutrition after the BPD/DS (2 percent of patients). Since food only goes through about 40 percent of the small intestine, absorption is diminished and patients have to eat more protein and take more vitamin and mineral supplementation than with the other procedures.
Clinical Practice Guidelines
Another important development in the treatment of obesity is the development of clinical practice guidelines (CPG). These were developed in a collaborative effort of the American Society of Metabolic and Bariatric Surgery (ASMBS), The Obesity Society (TOS), and the American Association of Clinical Endocrinologists (AACE). They were written in 2008 and updated in 2013. The CPG detail the multidisciplinary approach to the care of people afflicted with severe obesity before and after surgery. This includes specific guidelines regarding appropriate vitamin and mineral supplementation after surgery. It is very important that patient’s surgical/medical teams are familiar with the guidelines and that they follow them. It is very important that patients familiarize themselves with what the recommendations are for appropriate supplementation, so they can be sure that what they are taking is recommended by the clinical practice guidelines.
What’s on the Horizon?
Gastric Plication
According to the recent CPG, this is an investigational or experimental procedure that involves rolling in (placating) the greater curve of the body of the stomach to provide restriction without a foreign body (band) or need for removal (VSG). It has been used in combination with the bandings to improve weight-loss.
Endoscopic Procedures
A number of endoscopic procedures are in development. Some involve placating the stomach much like a gastric plication. Others involve placing a plastic barrier lining (Endobarrier®) that keeps food from contacting the small intestines, so it cannot be absorbed there. There is also an intra-gastric balloon (BioEnterics®) designed to make the patient feel full with less food.
Neuromodulation
The vagus nerves are a primary communication pathway between the brain and the abdominal organs and control much of the activity of the stomach, intestine, and pancreas. The vagus nerves play a significant role in food processing and in signaling the feeling of fullness and in prolonging the absence of hunger through nervous control. Nueromodulation is an experimental device that involves the implantation of electrodes onto the stomach to block the vagus nerves (VBLOC®) (The FDA is currently reviewing this device for approval in the U.S.) powered by a battery that is implanted under the skin of the abdominal wall.
The ASMBS’ position states, “The use of novel technologies should be limited to clinical trials done in accordance with the ethical guidelines of the ASMBS and designed to evaluate the risk and efficacy of the intervention.”
Conclusion
Bariatric surgery is the most appropriate treatment for the person affected by severe obesity. If you are considering bariatric surgery, it is important that you consult with a bariatric surgeon regarding your options. To locate a surgeon in your area, please visit www.ASMBS.org. If you are a post-surgery patient, it is important to follow-up with a multidisciplinary team and follow their recommendations regarding diet, exercise and supplementation.
About the Author:
Stephen Boyce, MD, obtained his Bachelor of Science and Masters of Science from Texas A&M University, College Station, before beginning medical school in Dallas, Texas at the University of Texas Southwestern Medical School where he received his medical degree. Surgical Residency was performed at Parkland Memorial Hospital in Dallas where he completed his general surgery training. With more than 24 years of experience performing bariatric surgeries, Dr. Boyce has completed more than 4,000 bariatric surgical procedures, has special training in advanced laparoscopic surgery and has also completed a Masters Certification in Bariatric Surgery. He started his own practice, the New Life Center for Bariatric Surgery, in Knoxville, Tenn. in 2002, which shortly after became one of the Nation’s first Centers of Excellence (7th in the Nation) in 2005. His special interest in bariatric nutrition led him to develop Bari Life Bariatric Supplements, specializing in custom multivitamin formulas for the bariatric surgery patient. Additionally, he is an active educator for Ethicon-Endo Surgery and a two-time recipient of the OAC’s “Dr. Blackstone Outstanding Membership Recruitment by a Physician” award.
by Kendall Griffey, OAC Communications Manager Spring 2024 We have officially kicked off Your Weight Matters Regional…
Read ArticleTelemedicine became a popular tool during the pandemic because it allows healthcare professionals to provide medical care…
View Videoby Kendall Griffey, OAC Staff; and Chrystal Jones, OAC Staff Fall 2022 For over ten years, the…
Read Article










